Artigo europeu, mas com foco nas nossas dificuldades de como implementar um programa de controle de germes gram negativo multiR em um cenário de restrição orçamentária (cada vez maior).
infecção hospitalar
OMS publica novas diretrizes para acabar com infecções cirúrgicas
Atualmente, em países de baixa e média renda, 11% dos pacientes que passam por cirurgias são infectados no procedimento. Nos Estados Unidos, complicações operatórias causadas por microrganismos ger…
Fonte: OMS publica novas diretrizes para acabar com infecções cirúrgicas
Doctors and Nurses: Wash Your Hands!

If our behavior changes when light, or attention, is shone on it, this is called the ‘Hawthorne effect’ — and it is alive and well in our approach to handwashing, says Dr Lundberg.
Fonte: Doctors and Nurses: Wash Your Hands!
Campanha do Medscape. Quem sabe em inglês a turma acredite…
Bacteria Can Persist on Gloves, Transfer to Surfaces

Acesse a reportagem do Medscape aqui
A bactéria em questão é o Acinetobacter balmani, figurinha carimbada dos serviços de controle de infecção hospitalar.
Vídeo: Como bactérias multiR se transmitem em hospitais
Fácil de entender como bactérias multirresistentes se disseminam em hospitais. Mais uma dica do meu amigo Dr. Arnaldo Gouveia Jr de Americana.
Empiric Piperacillin-Tazobactam versus Carbapenems in the Treatment of Bacteraemia Due to Extended-Spectrum Beta-Lactamase-Producing Enterobacteriaceae | Read by QxMD
Extended-spectrum beta-lactamase (ESBL)-producing Enterobacteriaceae are a common cause of bacteraemia in endemic countries and may be associated with high mortality; carbapenems are considered the drug of choice. Limited data suggest piperacillin-tazobactam could be equally effective. We aimed to compare 30-day mortality of patients treated empirically with piperacillin-tazobactam versus a carbapenem in a multi-centre retrospective cohort study in Singapore. Only patients with active empiric monotherapy with piperacillin-tazobactam or a carbapenem were included. A propensity score for empiric carbapenem therapy was derived and an adjusted multivariate analysis of mortality was conducted. A total of 394 patients had ESBL-Escherichia.coli and ESBL-Klebsiella pneumoniae bacteraemia of which 23.1% were community acquired cases. One hundred and fifty-one received initial active monotherapy comprising piperacillin-tazobactam (n = 94) or a carbapenem (n = 57). Patients who received carbapenems were less likely to have health-care associated risk factors and have an unknown source of bacteraemia, but were more likely to have a urinary source. Thirty-day mortality was comparable between those who received empiric piperacillin-tazobactam and a carbapenem (29 [30.9%] vs. 17 [29.8%]), P = 0.89). Those who received empiric piperacillin-tazobactam had a lower 30-day acquisition of multi-drug resistant and fungal infections (7 [7.4%] vs. 14 [24.6%]), P<0.01). After adjusting for confounders, use of empiric piperacillin-tazobactam was not associated with increased 30-day mortality (OR 1.00, 95% CI; 0.45-2.17). Empiric piperacillin-tazobactam was not associated with increased 30-day mortality and may result in fewer multi-drug resistant and fungal infections when compared with a carbapenem.
Ceftazidima/avibactam aprovada também na União Europeia
INFECÇÃO OCULAR – BRASIL (02) (SÃO BERNARDO DO CAMPO, SÃO PAULO), SURTO, POS-CIRURGIA DE CATARATA, PSEUDOMONAS, ATUALIZAÇÃO, FALHA EM PROCESSO DE TRABALHO
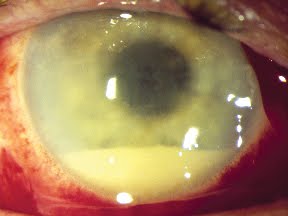
Já tínhamos compartilhado um post sobre esse assunto. Agora a conclusão da investigação de que os procedimentos cirúrgicos foram feitos sem um mínimo de cuidado com a esterilização e antissepsia.
A Randomized Trial Comparing Skin Antiseptic Agents at Cesarean Delivery

Disponível aqui (via QxMD read)
Protocolo de neutropenia febril
Conforme prometido aos alunos da enfermaria, posto este artigo que (apesar de ser de 2006) é bastante didático na sistematização do manejo clínico do paciente neutropênico febril.



 acesse via facebook
acesse via facebook
