Fonte: Quais doenças podem voltar ou avançar em 2019 no Brasil?
Mês: dezembro 2018
Fluoroquinolone Antibiotics: Safety Communication – Increased Risk of Ruptures or Tears in the Aorta Blood Vessel in Certain Patients
FDA review found that fluoroquinolone antibiotics can increase the occurrence of rare but serious events of ruptures or tears in the main artery of the body, called the aorta. These tears, called aortic dissections, or ruptures of an aortic aneurysm can lead to dangerous bleeding or even death. They can occur with fluoroquinolones for systemic use given by mouth or through an injection.
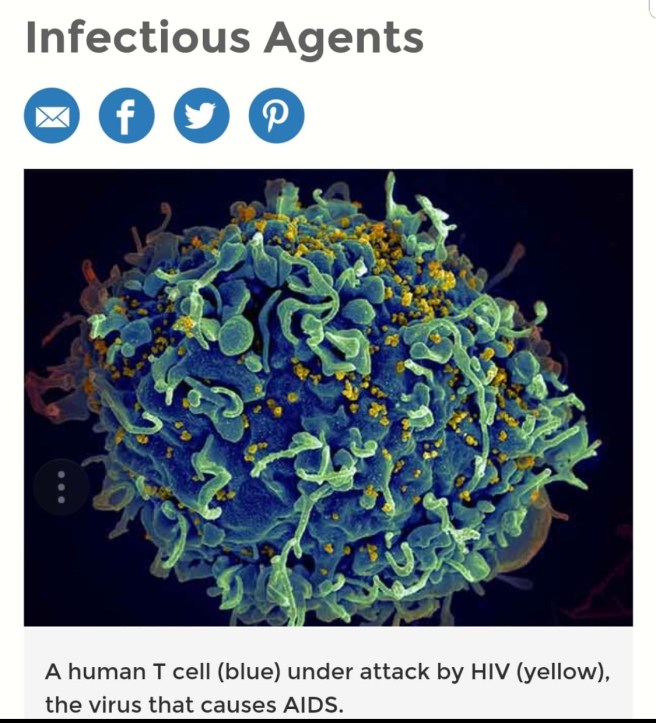
More than 3,000 patients at New Jersey surgery center possibly exposed to HIV, hepatitis
The patients may have been exposed to blood-borne illnesses due to “lapses in infection control in sterilization,” according to the surgery center.
Fonte: More than 3,000 patients at New Jersey surgery center possibly exposed to HIV, hepatitis
Risk of Herpes Zoster Prior to and Following Cancer Diagnosis and Treatment: A Population-Based Prospective Cohort Study.

Background: Information on the risks of herpes zoster (zoster) preceding a cancer diagnosis and the role of cancer treatment on risk is limited.
Methods: This was a prospective cohort of 241497 adults, with mean age 62.0 years at recruitment (2006-2009), linked to health datasets from 2006 to 2015. The relation between cancer diagnosis, treatment, and zoster risk was analyzed using time-varying proportional hazards models.
Results: Over 1760 481 person-years of follow-up, 20286 new cancer diagnoses and 16350 zoster events occurred. Participants with hematological and solid cancer had higher relative risks of zoster than those without cancer (adjusted hazard ratio [aHR], 3.74 [95% confidence interval {CI}, 3.11-4.51] and 1.30 [95% CI, 1.21-1.40], respectively). Compared to those without cancer, zoster risk was also elevated prior to a hematological cancer diagnosis (aHR for 1-2 years prior, 2.01 [95% CI, 1.31-3.09]), but this was not the case for solid cancers (aHR for 1-2 years prior, 0.90 [95% CI, .75-1.07]). Compared to those without cancer, zoster risk among participants with solid cancers receiving chemotherapy was greater than in those without a chemotherapy record (aHR, 1.83 [95% CI, 1.60-2.09] and 1.16 [95% CI, 1.06-1.26], respectively).
Conclusions: For hematological cancer, increases in zoster risk are apparent in the 2 years preceding diagnosis and treatment; for solid organ cancers, the increased risk appears to be largely associated with receipt of chemotherapy.
Seven versus fourteen Days of Antibiotic Therapy for uncomplicated Gram-negative Bacteremia: a Non-inferiority Randomized Controlled Trial.
![]()
Background: Gram-negative bacteremia is a major cause of morbidity and mortality in hospitalized patients. Data to guide the duration of antibiotic therapy are limited.
Methods: Randomized, multicenter, open-label, non-inferiority trial. Inpatients with Gram-negative bacteremia, afebrile and hemodynamically stable for at least 48 hours, were randomized to receive 7 (intervention) or 14 days (control) of covering antibiotic therapy. Patients with uncontrolled focus of infection were excluded. The primary outcome at 90 days was a composite of all-cause mortality; relapse, suppurative or distant complications; and re-admission or extended hospitalization (>14 days). The non-inferiority margin was set at 10%.
Results: We included 604 patients (306 intervention, 298 control) between January 2013 and August 2017 in three centers in Israel and Italy. The source of the infection was urinary in 411/604 (68%); causative pathogens were mainly Enterobacteriaceae (543/604, 90%). A 7-day difference in the median duration of covering antibiotics was achieved. The primary outcome occurred in 140/306 (45.8%) patients in the 7 days group versus 144/298 (48.3%) in the 14 days group (risk difference [RD] -2.6%, 95% confidence interval [CI] -10.5% to 5.3%). No significant differences were observed in all other outcomes and adverse events, except for a shorter time to return to baseline functional status in the short therapy arm.
Conclusions: In patients hospitalized with Gram-negative bacteremia achieving clinical stability before day 7, an antibiotic course of 7 days was non-inferior to 14 days. Reducing antibiotic treatment for uncomplicated Gram-negative bacteremia to 7 days is an important antibiotic stewardship intervention. (ClinicalTrials.gov number, NCT01737320).
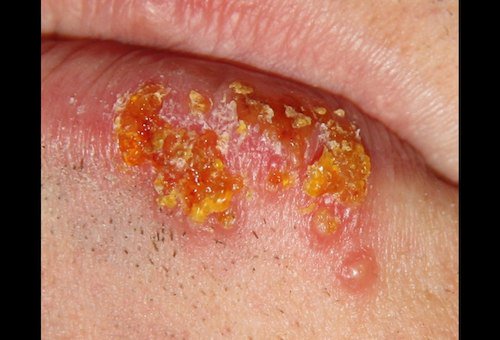
Herpesviruses: Test Your Knowledge
Prompt recognition of herpes simplex infection and early initiation of therapy are of utmost importance in the management of the disease. Test your knowledge of HSV and other herpesviruses.
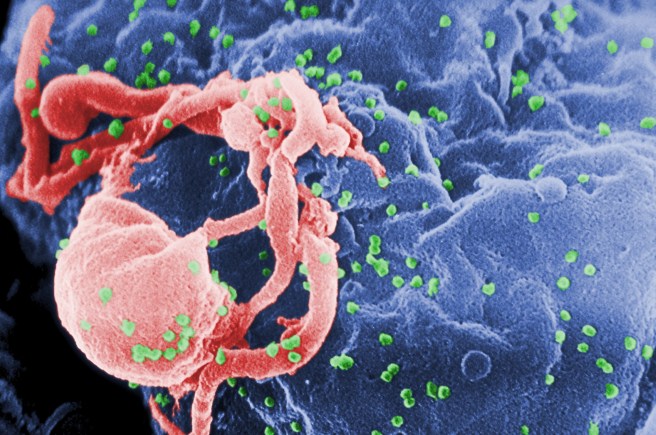
Imagem: HIV atacando um linfócito CD4
Agência Europeia faz severa advertência sobre o risco de quinolonas e entidades científicas brasileiras repercutem

Desafios na luta contra o sarampo podem fazer Brasil perder certificado de erradicação em 2019
País teve mais de 10 mil casos da doença em 2018. Baixa cobertura vacinal é problema no combate a novos casos.
Fonte: Desafios na luta contra o sarampo podem fazer Brasil perder certificado de erradicação em 2019
Vacina contra o HIV é testada com sucesso em macacos
Pesquisadores afirmam ter neutralizado a forma viral mais comum nas infecções do HIV em humanos